
ABSTRACT -Seborrheic dermatitis is a papulosquamous disorder patterned on the sebum-rich areas of the scalp, face, and trunk. In addition to sebum, this dermatitis is linked to Malassezia furfur. and some other causes. This article deal with an overview of seborrheic dermatitis focusing upon its various aspect along with homoeopathic management.
Methods– various literature and journals about seborrheic dermatitis and their homoeopathic approach are reviewed.
Conclusion- helps to understand the scope of homoeopathy in treating the symptoms and improving quality of life of patients suffering from seborrheic dermatitis .
Keynotes- seborrheic dermatitis ,dandruff, cosmetic issue ,homeopathy
INTRODUCTION– Seborrheic dermatitis (SD) is a common ,non contagious ,inflammatory skin disease presented with red patches and greasy scales on affected areas along with white or yellow crusty or powdery flakes , particularly the scalp, face, and body. SD can affect the scalp as well as other seborrheic areas, and involves itchy and flaking or scaling skin, inflammation and pruritus.1
EPIDEMIOLOGY—The worldwide prevalence of seborrheic dermatitis is around 5%, but the prevalence of its non-inflammatory variant, dandruff, is probably closer to 50%. SD affects all ethnic groups in all regions globally. 2 The prevalence of SD is bimodal with a peak in the first three months of life and then from adrenarche to a second peak after the fourth decade. It is slightly more common in men, but affected women tend to have more severe symptoms. SD also higher in HIV positive patients and other immunodeficiency disorder.
ETIOLOGY
SD is a multifactorial skin disease that needs endogenous and exogenous predisposing factors for its development. The fact that SD is more common in men and that, except in infants, it begins to develop at puberty, suggests a significant hormonal influence, mainly of androgens..
Genetic predisposition –in suspected because it runs in families
Immunodeficiency -because SD Frequently an initial manifestation in HIV positive patients.
The use of varying terms such as sebopsoriasis, seborrheic dermatitis, seborrheic eczema, dandruff, and pityriasis capitis reflects the vast clinical spectrum of SD and the controversy regarding its etiology3
PATHOLOGY–
Diagnosis of SD is typically made by history and physical examination. In rare cases, a skin biopsy is needed for differential diagnosis. Histologically, the development of SD can be divided into two stages. In the acute and sub-acute stages, SD shows superficial perivascular and perifollicular inflammatory infiltrates, composed mainly of lymphocytes and histiocytes in association with spongiosis and psoriasiform hyperplasia, and can be coupled with parakeratosis around follicular opening (“shoulder parakeratosis”).4
Patterns
Severe pattern recognized5
- Infantile SD
- Adult SD
- SD in patient with HIV infection
Infantile seborrheic dermatitis (ISD) is a chronic, inflammatory, scaling skin condition, which causes redness and a greasy scaling rash in infants and young children. It can last from weeks to months, but rarely years. When it occurs on the scalp, it is referred to as ‘cradle cap’.
Adult SD
Several site involved and several patterns recognized
SCALP—
Dandruff usually earliest and only manifestation of SD in most cases.
DANDRUFF
Dandruff is often defined as increased scaling of the scalp, representing the more active end of physiological desquamation. The postulate of fatty acid metabolism by the commensal lipophilic yeast of scalp skin.
FACE
Distribution characteristically involves medial part of eyebrows, glabella and nasolabial folds, may extends to other parts of face.
TRUNK
Severe pattern of SD recognized on trunk
Petaloid pattern
Commoner variant
Morphology: non exudative ,scaly annular /circinate lesions with follicular papules surmounted with greasy scales.
Pityriasiform pattern
Rarer
Morphology: extensive erythematous plaque surmounted with greasy yellow scales.
Distribution: trunk and neck, up to hair margin
Seborrheic folliculitis–
Rarer
Morphology: extensive erythematous folliculocentric papules surmounted with pustules
Distribution : trunk, usually back
flexures
Morphology: interitigo ,ill defined erythematous plaques surmounted with greasy scales .crusted fissures develop in the folds. secondary infection and frank eczematization common
Distribution: axillae ,groin ,inframammary areas umbilicus ,genitals ,and nasal cleft
SD in HIV positive patient
Most common dermatitis in AIDS patients.
Florid lesions with intense erythema , thick scales and involving unusual sites.
Cutaneous eruptions are commonly seen in acquired immunodeficiency syndrome (AIDS). Seborrheic dermatitis in this patient population is usually more severe and difficult to diagnose and treat.
Site of predilection- It most often occurs on the scalp and face, especially at the nasolabial folds, eyebrows, and forehead.
Course – the disease runs a chronic course with relapses and remissions.
Complications-
Superadded bacterial infections (in the scalp)
Candidal infection ( in the flexure)
Investigations-
Usually, no investigations are needed
Rule out HIV infection in patients with SD which is extensive ,severe, recurrent and recalcitrant to treatment.
DIAGNOSIS OF SD
Points for diagnosis
Diagnosis is based on
Morphology-folliculocentric lesion/flexural plaque surmounted with typical yellow ,greasy scales
Typical distribution seborrheic distribution
Differential diagnosis
Differential diagnosis of seborrheic dermatitis and dandruff.
| Diagnosis | Diagnostic Clues | |
| Psoriasis | Usually involves extensor, palmar, plantar, nails and extensor areas. Thick plaques sharply limited with silvery white scales. Positive family history | |
| Atopic Dermatitis | First appearance after 3 months of age, pruritus and restlessness are common. Frequently involves scalp, cheeks and extensor areas. | |
| Tinea Capitis | Commonly seen in children, frequently accompanied by hair loss patches with “black dots” (broken hair). Highly contagious. KOH examination of the hair shaft and fungal culture confirm the diagnosis. | |
| Rosacea | Usually targets the face. Papulopustules and telangiectasias on the malar, nose and perioral regions with slight desquamation.. | |
| Systemic Lupus Erythematous (SLE) | In acute stage, butterfly rash on face that spares the nose bridge or nasolabial folds. Photosensitivity is common. Skin lesions are generally associated with other clinical signs of SLE. Histology and serologic tests such as antinuclear autoantibodies confirm the diagnosis. | |
| Others | Pemphigus Foliaceous | Erythema, scaling and crusting that first present on the scalp and face can expand to chest and back.. |
| Pityriasis Rosea | Abrupt onset, appearance of herald patch and resolution within weeks. | |
| Secondary syphilis | Peripheral lymph-adenopathy, mucosal lesions and palmoplantar macula-papules. Serology tests such as VDRL/ RPR, FTA-ABS* confirm diagnosis. | |
| Diaper Dermatitis | lower abdomen, genitalia, buttocks and upper thighs. Spares skin folds. Pustules are common. | |
| Langerhans cell histiocytosis | Multisystem disease. Brown to purplish papules prone to coalesce on the scalp, retro-auricular areas, axillae and inguinal folds. |
HOMOEOPATHIC APPROACH 6,7 —
Homeopathy works wonderfully well in treating seborrheic dermatitis. These medicine treat both acute and chronic seborrheic dermatitis effectively
Sulphur-dry, scaly, unhealthy. Itching ,burning; worse scratching and washing. pruritus especially from warmth, in the evening often recurs ,in damp weather.
Nat mur– Eczema ; raw , red ,inflamed , especially in edge of hair; <from eating too much salt , at sea shore , or ocean voyage.
Kali Sulph-Eczema ; burning ,itching, popular eruption. Nettle Rash. Seborrhea. Ring worm of scalp or beard with abundant scales.
Mezerium– Eczema ; intolerable itching ; chilliness with pruritus; worse in bed. Eruptions ulcerate and form thick scabs under purulent matter exudes.
Sepia-itching ; not relieved by scratching ; worse in bends of elbows and knees. Ringworm –like eruptions every spring.
Psorinum– Scalp ; dry or moist . foetid , suppurating eruptions; oozing a sticky ,offensive fluid . Intolerable itching . Sebaceous glands secrete excessively . Oily skin crusty eruptions all over. Eczema behind ear.
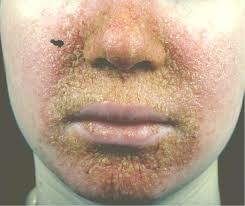
Seborrheic dermatitis8
REFERENCES
1.Borda LJ, Wikramanayake TC. Seborrheic Dermatitis and Dandruff: A 1044.1000019. doi: 10.13188/2373-1044.1000019. Epub 2015 Dec 15. PMID: 27148560; PMCID: PMC4852869
2.Tucker D, Masood S. Seborrheic Dermatitis. [Updated 2022 May 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-.
3.Clio Dessinioti, Andreas Katsambas,Seborrheic dermatitis: Etiology, risk factors, and treatments:: Facts and controversies,Clinics in Dermatology,Volume 31, Issue 4,2013,
4.Wikramanayake TC, Borda LJ, Miteva M, Paus R. Seborrheic dermatitis-Looking beyond Malassezia. Exp Dermatol. 2019 Sep;28(9):991-1001. doi: 10.1111/exd.14006. Epub 2019 Aug 19. PMID: 31310695.
5.Khanna N,Illustratred Dermatology and Sexually Transmitted Disease, 5th Edition,Elsevier India Pvt Ltd, New Delhi, India (2004).
6. Allen HC. Keynotes and characterstics with comparisons of some of the leading remedies of the materia medica with bowel nosodes. Reprint Edition. B. Jain Publishers (P) Ltd, New Delhi, India (2004).
7.Boericke W. Pocket manual of homoeopathic materia medica and repertory. (51st Impression), B. Jain Publishers (P) Ltd, New Delhi, India (2011).
8.B. Cribier, C. Taieb, M. Saint Aroman, J. Shourick, SARS‐CoV‐2: skin diseases, mask wearing and unpleasant sensations, Journal of the European Academy of Dermatology and Venereology, 10.1111/jdv.17380, 35, 9, (e558-e560), (2021).
About Authors:-
Dr. Shruti Patel
M.D. (2020 Batch)
Dr. Sana khan
M. D. (2019 Batch)
State National Homoeopathic Medical College & Hospital
Lucknow




