ABSTRACT
Dyspepsia is a constellation of symptoms referable to the gastroduodenal region of the upper gastrointestinal tract. Functional dyspepsia is a remitting and relapsing disorder and one of the most common causes of these symptoms [1]. It is a common disorder of gut-brain interaction, with most patients managed in primary care [2]. The community prevalence of dyspepsia ranges from 20% to 40% and causes 3% to 5% pf primary care visits [3]. Functional dyspepsia is diagnosed when an organic aetiology for the symptoms is not identified. Treatment options available in modern medicine are varied; however, the evidence supporting the therapies is weak, and the response rate is less.
This article defines functional dyspepsia, its risk factors, discusses possible pathophysiologic mechanisms, evaluation of the disorder and its Homoeopathic management.
DEFINITION AND CLINICAL PRESENTATION
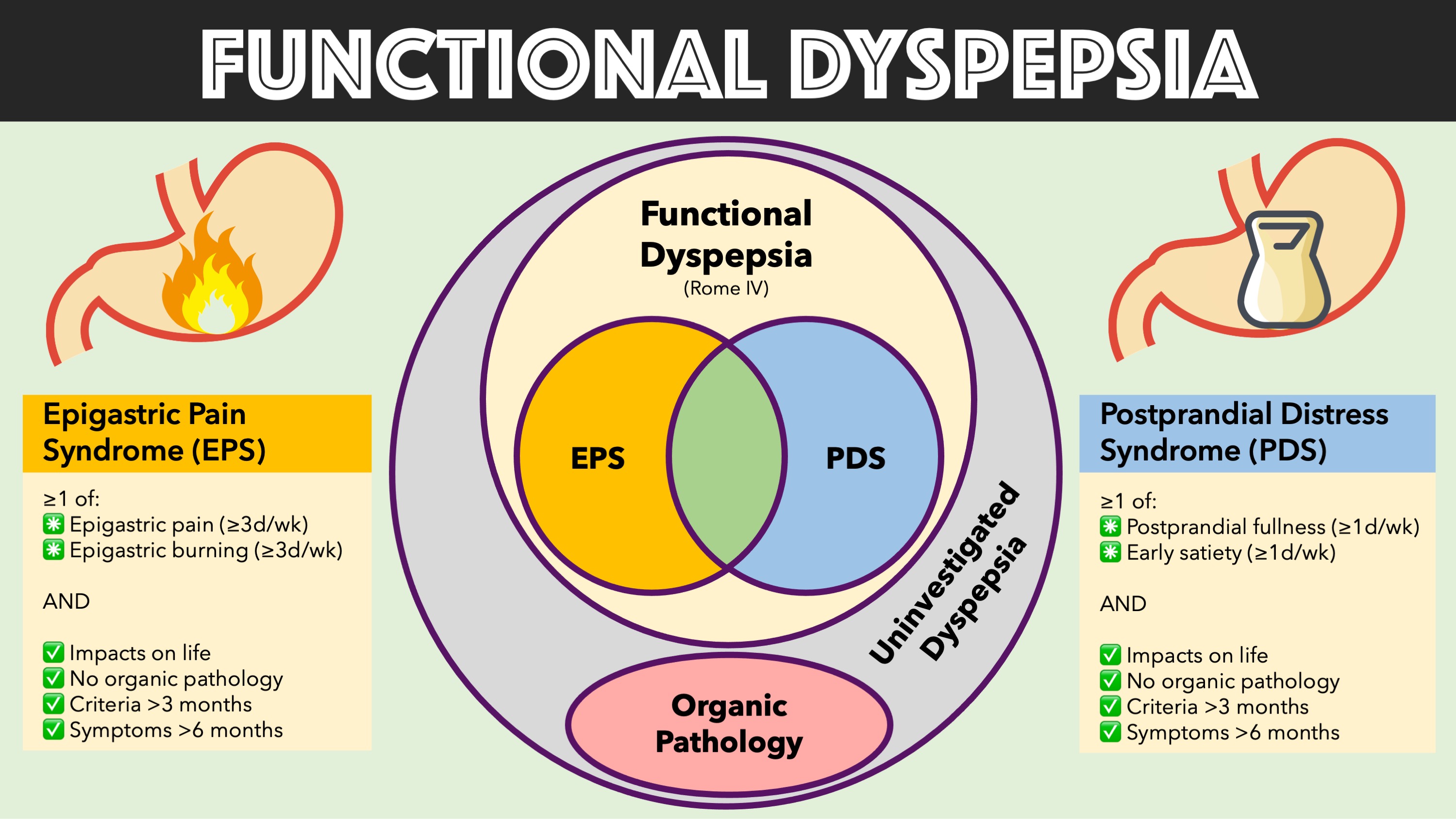
Dyspepsia symptoms include symptoms of upper gastroduodenal complaints, such as belching, postprandial fullness, early satiety, epigastric pain, and epigastric burning. Functional dyspepsia is diagnosed when and organic aetiology for the symptoms is not identified. Functional dyspepsia is defined by Rome IV criteria and further classified into postprandial distress syndrome and epigastric pain syndrome. The epigastric pain syndrome consists of intermittent pain or burning in the epigastrium, occurring at least once per week, and the postprandial distress syndrome is marked by the occurrence of at least several times per week of bothersome postprandial fullness occurring after normal-sized meals or by early satiety that prevents the person from finishing the regular meal.
PATHOPHYSIOLOGY
Despite extensive research, and due to both its multifactorial nature and the heterogeneity of symptoms, the underlying pathophysiology of functional dyspepsia remains unclear. In recent decades many systematic pathophysiological studies comparing functional dyspepsia patients with healthy persons have demonstrated that functional dyspepsia is an organic disorder, which includes motility disorders, sensorimotor dysfunction connected hypersensitivity to mechanical and chemical stimuli, immune activation, elevated mucosal permeability in the proximal small intestine and disorders of autonomic and enteric nervous systems. Along with the mentioned causes psychological stress, particularly anxiety is associated with functional dyspepsia and may precede the onset of the disorder in some persons. Infections may cause functional dyspepsia, but the evidence is not well established. Duodenal inflammation has been observed in up to 40% of patients with functional dyspepsia particularly subtle duodenal eosinophilia.
RISK FACTORS
Numerous epidemiological studies demonstrate that female gender, smoking, use of NSAIDs, and H. pylori infection are associated with dyspepsia in the community, but the evidence of these associations is not very large. Higher body mass index was an independent predictor of development of functional dyspepsia in one longitudinal study. One multi-ethnic study in Malaysia reported a significantly higher prevalence of functional dyspepsia in Indian and Malay participants, compared with Chinese. Psychological co-morbidity plays a major role in the development of functional dyspepsia, particularly as the gut and brain communicate through the enteric nervous system and the hypothalamic-pituitary-adrenal axis [HPAA]. In a Swedish population-based survey, anxiety led to an almost eight-fold increased odds of developing functional dyspepsia over a 10-year period. Two Australian longitudinal studies demonstrated bi-directional effects between gut and brain; individuals with functional dyspepsia at baseline were more likely to develop anxiety or depression during follow-up and individuals with anxiety and depression at baseline were more likely to develop functional dyspepsia. Acute gastroenteritis is also associated with new onset of functional dyspepsia, termed post-infection functional dyspepsia. A meta-analysis of 19 studies reported an almost three-fold increased odds of developing functional dyspepsia in exposed individuals >6 months post-infection. Up to 80% of patients with functional dyspepsia report meal-induced symptoms, but the role of food in the development of functional dyspepsia is unclear.
MANAGEMENT
Management of functional dyspepsia includes reassurance that there is no structural cause for the symptom. There is little evidence that lifestyle changes or exercise led to symptoms improvement. Medical therapy is therefore the mainstay of treatment. Some of the Homoeopathic medicines that proves effective for the symptoms of dyspepsia are
ABIES CANADENSIS– Mucous membranes are affected and gastric symptoms are most marked, and a catarrhal condition of the stomach is produced. There are peculiar cravings and chilly sensations that are very characteristic. Tendency to eat far beyond capacity for digestion.
ABIES NIGRA- A long-acting remedy, in various forms of disease, whenever the characteristic stomach symptoms are present. Most of the symptoms are associated with gastric disturbances. In dyspeptic troubles of the aged, with functional heart symptoms, also after tea or tobacco. Pain in stomach always comes on after eating. Sensation of a lump that hurts, as if a hard-boiled egg lodged in the cardiac end of stomach.
ALETRIS FARINOSA- Disgust for food, least food causes distress. Nervous dyspepsia
ANGUSTURA VERA- Bitter taste. Irresistible desire for coffee. Pain from navel into sternum. Atonic dyspepsia. Belching with cough.
ANACARDIUM- Neurasthenics; such have a type of nervous dyspepsia. Weak digestion with fullness and distension. Empty feeling in stomach. Eating relieves the Anacardium dyspepsia.
ARGENTUM NITRICUM- Neurotic effects are very marked. Upper abdominal affections brought on by undue mental exertion. Very characteristic is the great desire for sweets, the splinter-like pains.
LYCOPODIUM- Adapted more especially to ailments gradually developing, functional power weakening, with failures of the digestive powers. Immediately after a lights meal abdomen is bloated, full.
NUX VOMICA- Nausea in the morning, after eating. Weight and pain in stomach; worse eating, some time after. Epigastrium bloated, with pressure as of a stone, several hours after eating. Dyspepsia from drinking strong coffee.
QUASSIA–PICRAENA EXCELSA- Acts on gastric organs as a tonic. Atonic dyspepsia, with gas and acidity. Heartburn and gastralgia. Dyspepsia after infectious diseases; especially grip, dysentery. Tongue dry or with brown sticky coating
ROBINIA- The remedy for hyperchlorhydria. The gastric symptoms with the most pronounced acidity are well authenticated, and are the guiding symptoms. The acidity of Robinia is accompanied by frontal headache.
About Author
Dr. Prajkta khanvilkar, MD Scholar, Batch 2020-21, Department of Practice of Medicine, Government Homoeopathic Medical College and Hospital, Bhopal, Madhya Pradesh




