Abstract :
The scrotal venous pampiniform plexus, which drains blood from each testicle, abnormally enlarges and dilates. This condition is known as a varicocele. Varicoceles are the most often found cause of poor sperm morphology, low sperm count, reduced sperm motility, and abnormal semen analysis. Despite being typically painless, varicoceles are clinically important. There are three sizes of varicoceles: small, medium, and giant. Although it is a surgical condition, homoeopathic medicines can be used to treat it. To handle the case using homoeopathic medications, it is important to track the case as soon as possible. Even in the case of surgical history, varicocele can be effectively avoided from recurring with knowledge of the condition and homoeopathic care.[1]
Keywords: homoeopathy, male infertility, scrotal venous pampiniform plexus, varicocele,
Introduction :
The scrotal venous pampiniform plexus, which drains blood from each testicle, abnormally enlarges and dilates. This condition is known as a varicocele. Varicoceles are the most often found cause of poor sperm morphology, low sperm count, reduced sperm motility, and abnormal semen analysis.
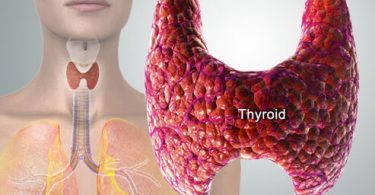
The pampiniform plexus is made up of the testicular veins that emerge from the testis. Later, venous blood that is a portion of the spermatic cord ascends via the inguinal canal to create the internal spermatic or testicular vein, which empties into the abdomen. The internal spermatic vein on the right connects the left renal vein on the left side, where it ends into the low-pressure inferior vena cava. This anatomy explains why the left side has the highest percentage of clinically visible varicoceles.
Based on their clinical appearance and visible size, varicoceles are divided into three categories: small, medium, and massive. [1,2]
Epidemiology :
15% to 20% of all adult males have varicoceles, while 40% of infertile males have them as well. Although there are several theories, it is unclear exactly how a varicocele affects sperm production, structure, and function. But there is no denying the link between clinically significant varicoceles and male infertility. British physician Barfield initially noticed this connection in the late 1800s, and other people later corroborated it in the early 1900s.[3]
Etiology :
Although the exact cause of varicoceles is unknown, it is believed to result from a venous blood flow backup in the internal spermatic vein, which results in venous engorgement that can be clinically seen on scrotal examination. In the left testicle, varicoceles are much more common (80% to 90%). There is a 30% to 40% chance that a left varicocele is a bilateral issue if it is found. As for the anatomical reason, there are three possibilities:
A) The left internal spermatic vein becomes impaled between the superior mesenteric artery and the aorta, resulting in the “Nutcracker” effect. Vein compression and spermatic vein blockage are brought on by this entrapment.
B) Failure of the anti-reflux valve at the junction of the left renal vein and the internal spermatic vein. The testicular vein experiences reflux and retrograde flow as a result of this failure.
C) Angulation where the left renal vein and internal spermatic vein meet.
Deep vein thrombosis, renal arteriovenous malformations, and pampiniform plexus thrombosis are all uncommon causes of varicoceles.
Male infertility is made more likely by smoking tobacco and abnormalities in the gene that produces glutathione S-transferase Mu 1. These elements could also make you more likely to develop a varicocele.
On microscopic semen examination, a varicocele commonly results in a “stress pattern” when it contributes to an abnormal semen analysis. Low sperm counts, poor sperm motility, and a rise in the proportion of defective sperm make up this pattern. [4,5]
Pathophysiology :
- Infertility is typically the main worry with a varicocele. While many men with varicoceles are fertile, some also have sperm that is defective in terms of movement, morphology, quantity, or function. As a result of increased oxidative stress brought on by blood pooling that results in decreased oxygenation, direct hydrostatic pressure injury effects on the testis, toxin production, hypoxia, autoimmunity, or an increase in the concentration of adrenal steroids being delivered to the testicle, researchers theorise that the sperm may be damaged. This is because the adrenal veins empty into the left renal vein almost directly across from where the internal spermatic vein enters. The most widely recognised explanation for reduced sperm in varicoceles is that increased blood flow causes greater intratesticular temperature.
- Untreated varicoceles may advance, but they rarely hurt even when they do. Increased testicular temperatures, higher venous pressure, oxidative stress, hormonal imbalances, toxic metabolite reflux from the kidneys or adrenals, hypoxia, or potential stretching of nerve fibres in the spermatic cords from the dilated varicocele complex are some suggested mechanisms for such pain. Varicoceles-related orchialgia is frequently reported as aching, dull, or throbbing, although it is extremely uncommon for discomfort to be severe, sharp, or stabbing.
- Large varicoceles are expected to eventually lead to testicular failure, which may then result in decreased hormone synthesis, oligospermia, and testicular atrophy. Additionally, varicoceles have been associated with decreased sperm motility, viability, counts, and abnormal morphology.
- The Leydig cells in the testes may produce less testosterone as a result of varicoceles. In more than 80% of patients, varicocelectomy improves blood testosterone levels, with a mean improvement of between 100 and 140 ng/mL. Men with hypogonadal levels of testosterone (˂300 ng/mL) had the highest increases in testosterone. According to this research, varicocelectomy may be a good surgical option for hypogonadal males with severe varicoceles to permanently address low testosterone levels.[6,7,8]
Clinical manifestations :
- Varicoceles often have no symptoms.
- If the varicocele is big enough, the patient could describe it as a “bag of worms”.
- Varicoceles typically appear as soft lumps on the left side of the scrotum, above the testicle.
- Varicoceles on both the right and left sides are also possible.
- Patients may report feeling heavy or in discomfort in the scrotum. They are frequently discovered during an examination for infertility.
Large varicoceles will typically have the “bag of worms” look and are easily recognised by basic visual inspection.
Medium varicoceles are those that may be felt or seen during a physical examination without the patient pushing down on them.
Small varicoceles are those that can only be seen under a strong Valsalva (bearing down) manoeuvre.[3]
Infertility, reduced testicular atrophy, and discomfort reduction are reasons to have a varicocele removed. Candidates for repair satisfy the requirements listed below:
- Male infertility, normal fertility in females (however male varicocele treatment is not contraindicated in females with female infertility causes)
- Varicole that may be felt
- Semen parameters that are abnormal (“stress pattern”)
- suffering from varicocele pain.[7]
Investigations :
- After a physical examination, a high-resolution colour-flow Doppler ultrasound can be used to confirm the presence of varicocele. This ultrasound will show dilated pampiniform plexus vessels, typically larger than 3 mm in diameter. Venography is unnecessary.[9]
- Another painless, non-contact, non-invasive method for assessing and confirming a potential varicocele is thermal imaging.[10]
- The potential use of testicular strain elastography in locating varicocele patients who would benefit from therapy is being investigated.[11]
- Any isolated right-sided varicocele should always be suspected to be caused by renal cell carcinoma. A right-sided varicocele and venous blockage caused by a tumour thrombus in the right renal vein that can extend into the vena cava. CT scan is advised if this is thought to be feasible.[12]
Homoeopathic remedies for management of varicocele :
The choice of remedy should be made in accordance with how closely the patient’s symptoms match those of the remedy, as homoeopathy operates under the Similia Similibus Curantur principle. Here are a few significant homoeopathic medications with a list of associated symptoms:-[13,14,15,16,17]
- Aesculus hippocastanum – Generally slowed down, with purple varicose veins and venous stasis. Various areas of fullness, dryness, and swollen mucous membranes. Prostatic fluid passing through the stool.
- Aristolochia clematis – Prostatitis and epididymitis affecting male genitalia. Varicocele, worse from cold.
- Arnica montana – Especially well-suited to situations where any damage, no matter how slight, appears to have contributed to the current issue. Strains result from overusing any organ after catastrophic damage. Bruised, limp, and in pain.
- Aurum metallicum – Testicular pain and swelling. testicular induration that is persistent. brutal erections. testicular atrophy in boys.
- Calcarea fluorica – A potent tissue treatment for swollen, varicose veins, and hard, stony glands. Testicular induratures; hydrocele. Varicocele.
- Collinsonia canadensis – Constriction and a feeling of weight. Engorgement of the veins. Even worse, cold from even the smallest mental excitement or emotion. Heat is better. Varicocele associated with rectal symptoms.
- Fluoricum acidum – Complaints about weak, swollen blood arteries in older people or prematurely aged people. Urine is burning. Erections at night while sleeping enhanced sexual arousal and desire. Enlarged scrotum. Varicocele.
- Hamamelis virginiana – The focus of this treatment seems to be venous congestion, haemorrhages, varicose veins, and haemorrhoids with bruised pain of the afflicted areas. acts on the vein coatings, inducing relaxation and engorgement as a result. Spermatic cord pain that spread to the testicles. Varicocele. male testicles hurt. Orchitis. swollen, uncomfortable, and heated testicles. Epididymitis.
- Lachesis mutus – Tension felt in many places. Nothing tight anyplace is bearable.intense arousal of the sexual organs.
- Lycopodium clavatum – Impotence; the absence of erection. Emission that is premature. expand prostate size. Condylomata.
- Medorrhinum – Night time emissions, then extreme weakness. Impotence. Gleet; urethra as a whole feels painful. Urethritis. Prostate that is enlarged and uncomfortable, with frequent urges and difficult urination.
- Mercurius iodatus ruber – Especially on left side, with much glandular swelling.
- Nux vomica – Testicular discomfort that is constricted. Orchitis. Spermatorrhoea, along with nightmares, back pain, a burning sensation down your spine, weakness, and anger.
- Penthorum sedoides – Sexual ecstasy, erethism, and nearly satyriasis followed by a protracted period of sadness and impotence, varicocele.
- Phosphoricum acidum – Nocturnal emissions. Seminal vesiculitis. Lack of sexual arousal; painful and swollen testicles. During an embrace, parts relax, even while using a soft stool, prostatorrhea. Scrotal eczema. Prepuceal oedema and enlarged glans-penis. Preputial herpes. sycotic exudates.
- Plumbum metallicum – Testicles felt tight and pulled up.
- Pulsatilla pratensis – Testicles and abdomen both hurt from orchitis. urethral discharge that is thick and yellow; advanced gonorrhoea. Strictness; the urine stream was halted and just a few drops were passed, prostatitis acute. Tenesmus and pain when peeing, especially when laying on the back.
- Ruta graveolens – Complaints about flexor tendon or any muscular structure strain in particular.
- Silicea terra – Genital pain and burning, together with an eruption on the inner area of the thighs. recurring gonorrhoea with foul-smelling, heavy discharge. Elephantiasis of the testicles. nocturnal discharges; sexual erethism. Hydrocele.
- Sulphur – Feels as if needles in the penis. unintentional emissions. Genital itching before going to sleep. Cold, at ease, and helpless organs.
- Tabacum – Varicocele, frequent erections, prostatic fluid flow, nocturnal discharges until awakening, flabby genital organs, no erection or sexual desire.
References :
- Paick S, Choi WS. Varicocele and testicular pain: a review. The world journal of men’s health. 2019 Jan;37(1):4.
- Yetkin E, Ozturk S. Dilating vascular diseases: pathophysiology and clinical aspects. International Journal of Vascular Medicine. 2018 Aug 26;2018.
- Leslie SW, Sajjad H, Siref LE. Varicocele.
- Arafa M, Henkel R, Agarwal A, Majzoub A, Elbardisi H. Correlation of oxidation–reduction potential with hormones, semen parameters and testicular volume. Andrologia. 2019 Jun;51(5):e13258.
- Reesink DJ, Huisman PM, Wiltink J, Boeken Kruger AE, Lock TM. Sneeze and pop: a ruptured varicocele; analysis of literature, guided by a well-documented case-report. BMC urology. 2019 Dec;19(1):1-6.
- Vaganée D, Daems F, Aerts W, Dewaide R, van den Keybus T, De Baets K, De Wachter S, De Win G. Testicular asymmetry in healthy adolescent boys. BJU international. 2018 Oct;122(4):654-66.
- Cho CL, Esteves SC, Agarwal A. Indications and outcomes of varicocele repair. Panminerva Medica. 2019 Jun 1;61(2):152-63.
- Kohn TP, Ohlander SJ, Jacob JS, Griffin TM, Lipshultz LI, Pastuszak AW. The effect of subclinical varicocele on pregnancy rates and semen parameters: a systematic review and meta-analysis. Current urology reports. 2018 Jul;19:1-0.
- Hannick JH, Blais AS, Kim JK, Traubici J, Shiff M, Book R, Lorenzo AJ. Prevalence, doppler ultrasound findings, and clinical implications of the nutcracker phenomenon in pediatric varicoceles. Urology. 2019 Jun 1;128:78-83.
- Shakeri S, Malekmakan L, Manaheji F, Tadayon T. Inter-observer agreement on varicoceles diagnosis among patients referred to Shiraz Namazi Hospital. International Journal of Reproductive BioMedicine. 2018 Oct;16(10):649.
- Rocher L, Gennisson JL, Baranger J, Rachas A, Criton A, Izard V, Bertolloto M, Bellin MF, Correas JM. Ultrasensitive Doppler as a tool for the diagnosis of testicular ischemia during the Valsalva maneuver: a new way to explore varicoceles?. Acta Radiologica. 2019 Aug;60(8):1048-56.
- Hadad Z, Norup K, Petersen C. Right-sided varicocele testis as the only sign of right-sided renal tumour. Ugeskrift for Laeger. 2016 Feb 1;178(5):V05140307-.
- Boericke W. Pocket Manual of Homoeopathic Materia Medica & Repertory: Comprising of the Characteristic and Guiding Symptoms of All Remedies (clinical and Pahtogenetic [sic]) Including Indian Drugs. B. Jain publishers; 2002.
- Clarke JH. A dictionary of practical materia medica. New Delhi: B.
- Kent JT. Lectures on homoeopathic materia medica. New Delhi: B.
- Nash EB. Leaders in homoeopathic therapeutics. Boericke & Tafel; 1913.
- Phatak SR. Materia medica of homoeopathic medicines. B. Jain Publishers; 1999.